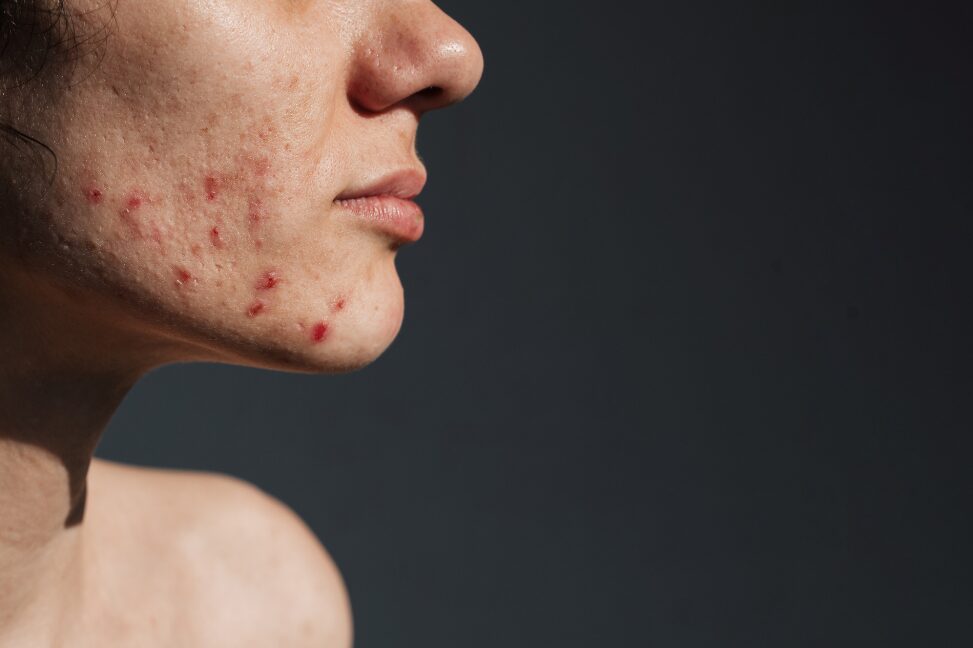
Holistic Skincare for Hormonal Acne: Your Guide to Clear Skin
Hormonal acne is a frustrating reality for many, extending far beyond the teenage years. Unlike occasional blemishes, these breakouts often feel relentless, deeply rooted, and significantly impact self-esteem. If you’ve found yourself searching for effective solutions and wondering, „Was tun gegen hormonelle Akne?“ (What to do about hormonal acne?), you’re not alone. This comprehensive guide will delve into the intricacies of hormonal acne, from its underlying causes and diverse manifestations to a holistic approach that truly addresses the issue for lasting clear skin.
Understanding hormonal acne isn't just about treating surface symptoms; it's about recognizing the intricate connection between your internal hormonal balance and your skin's health. By adopting a holistic perspective, we can unearth the root causes and implement a multi-faceted strategy for effective management and prevention.
Understanding Hormonal Acne: The Root Causes
At its core, hormonal acne is an inflammatory skin condition driven by fluctuations in your body's hormone levels. While both men and women produce a range of hormones, the balance between estrogens, progestogens, and androgens (like testosterone) significantly influences skin health. When this delicate equilibrium is disrupted, it can lead to a cascade of events that manifest as acne:
- Increased Sebum Production: Androgens, often referred to as "male hormones" but present in both sexes, stimulate the sebaceous glands to produce more oil (sebum). Excess sebum creates a fertile ground for bacteria and clogged pores.
- Inflammation: Hormonal shifts can trigger inflammatory responses in the skin, leading to red, painful lesions.
- Cell Turnover: Imbalances can affect how skin cells shed, leading to a buildup of dead skin cells that can further block pores.
Hormonal imbalances can be triggered by various factors and life stages:
- Puberty: A classic time for surges in androgens.
- Menstrual Cycle: Many women experience breakouts in the week leading up to their period due to fluctuating estrogen and progesterone levels. To learn more about these specific breakouts, you might find our article on Period Pimples: Understanding Hormonal Acne & How to Fight It particularly helpful.
- Pregnancy and Postpartum: Significant hormonal shifts can lead to acne flares.
- Stopping or Starting Birth Control Pills: Hormonal contraceptives regulate hormone levels; discontinuing them can lead to a rebound in androgen activity.
- Polycystic Ovary Syndrome (PCOS): A common endocrine disorder characterized by higher androgen levels, leading to acne, hirsutism, and irregular periods.
- Stress: Chronic stress can increase cortisol levels, which in turn can influence androgen production.
Hormonal acne commonly appears on specific areas of the face such as the jawline, chin, and around the mouth, often forming deep, cystic lesions. However, it's not limited to the face; areas like the back, neck, and chest can also be significantly affected.
Navigating the Landscape of Hormonal Acne Types
While the underlying cause is hormonal, acne manifests in different forms and severities. Recognizing the specific type of acne you're experiencing is crucial for tailoring an effective treatment plan.
Acne Vulgaris (Puberty Acne)
Often considered the most prevalent form, Acne Vulgaris, or puberty acne, impacts over 70% of adolescents between 15 and 18 years old. It's characterized by blackheads (comedones), whiteheads, and pustules, primarily affecting the face, back, and shoulders. The inflammation in this type generally remains in the upper layers of the skin, making it highly responsive to targeted skincare and over-the-counter treatments.
Acne Tarda (Adult-Onset Acne)
In contrast to its adolescent counterpart, Acne Tarda, or adult-onset acne, typically emerges much later in life, usually after the age of 25. Women are disproportionately affected by this form, largely due to hormonal fluctuations associated with life events such as discontinuing oral contraceptives, pregnancy, or perimenopause. Lesions often present as deeper papules, pustules, or even painful cysts, predominantly on the jawline, chin, neck, and torso. It can be particularly persistent and may require a more specialized approach.
Acne Conglobata (Severe Cystic Acne)
This is a particularly severe and chronic form of hormonal acne. Acne Conglobata involves deep, interconnected cysts and nodules that can be intensely painful. These lesions are typically found on the face, neck, back, and décolleté. Due to their depth and inflammatory nature, they often lead to significant scarring upon healing. While it can affect anyone, this severe form is more frequently observed in men. Given its severity and potential for lasting damage, immediate and aggressive medical intervention from a dermatologist is absolutely essential.
A Holistic Approach to Managing Hormonal Acne: Was Tun Gegen Hormonelle Akne?
When considering was tun gegen hormonelle Akne, a multi-pronged, holistic strategy is paramount. It’s not just about what you put on your skin, but also about supporting your body’s internal balance.
Targeted Skincare Strategies
Your daily skincare routine plays a vital role. The goal is to manage oil, reduce inflammation, and prevent pore blockages without irritating your already sensitive skin.
- Gentle Cleansing: Use a mild, pH-balanced cleanser twice daily. Harsh cleansers can strip the skin, leading to increased oil production and irritation.
- Strategic Actives: Incorporate ingredients known for their acne-fighting properties. Salicylic acid (BHA) penetrates oil to exfoliate within the pore. Benzoyl peroxide helps kill acne-causing bacteria. Retinoids (like adapalene or prescription tretinoin) normalize cell turnover, preventing clogged pores and reducing inflammation. Always introduce new actives slowly to avoid irritation.
- Hydration is Key: Even oily or acne-prone skin needs moisture. Choose a lightweight, non-comedogenic moisturizer to support the skin barrier. Dehydrated skin can produce more oil to compensate.
- Sun Protection: Many acne treatments increase sun sensitivity. Use a broad-spectrum SPF 30+ daily, opting for mineral formulations if chemical sunscreens cause irritation.
- Hands Off: Resist the urge to pick or squeeze pimples. This can worsen inflammation, spread bacteria, and lead to scarring.
- Consistency is Crucial: Skincare takes time. Give new products at least 6-8 weeks to show results before evaluating their effectiveness.
Nutritional & Lifestyle Adjustments
What you consume and how you live profoundly impacts your hormone health and, consequently, your skin.
- Anti-Inflammatory Diet: Focus on whole, unprocessed foods. Incorporate plenty of fruits, vegetables, lean proteins, and healthy fats (like omega-3s found in fish, flaxseed). These provide antioxidants and anti-inflammatory compounds.
- Mindful Eating: Consider reducing intake of high-glycemic foods (sugary drinks, refined carbs), dairy, and excessive red meat, which some studies suggest can exacerbate acne in certain individuals.
- Prioritize Gut Health: A healthy gut microbiome is linked to balanced hormones and reduced inflammation. Include probiotics (fermented foods) and prebiotics (fiber-rich foods) in your diet.
- Stress Management: Chronic stress elevates cortisol, which can drive androgen production. Practice stress-reducing techniques such as meditation, yoga, deep breathing exercises, or spending time in nature.
- Quality Sleep: Aim for 7-9 hours of quality sleep per night. Sleep is essential for hormone regulation and skin repair.
- Regular Exercise: Physical activity can help regulate hormones, reduce stress, and improve circulation, delivering nutrients to the skin.
- Stay Hydrated: Drinking plenty of water supports overall bodily functions, including skin health and detoxification.
When to Seek Professional Help
While lifestyle changes and targeted skincare are powerful, some forms of hormonal acne require medical intervention. If your acne is severe, persistent, painful, or causing scarring, it's time to consult a healthcare professional.
- Dermatologist: They can prescribe stronger topical medications (like prescription-strength retinoids), oral antibiotics to reduce bacteria and inflammation, or hormonal therapies such as spironolactone (which blocks androgen receptors) or oral contraceptives (which regulate hormone levels). Early intervention can prevent long-term scarring.
- Endocrinologist: If there’s a suspicion of an underlying hormonal disorder like PCOS, an endocrinologist can provide diagnosis and specialized management.
- In-Office Treatments: Procedures like chemical peels, microdermabrasion, or various laser therapies can be effective complements to your home routine, helping to reduce active breakouts and address post-inflammatory hyperpigmentation or scarring. For more detailed insights into effective remedies, explore our article on Hormonal Acne: Causes, Types & Effective Remedies.
Integrating Advanced Solutions and Ongoing Care
The journey to clear skin from hormonal acne is often a marathon, not a sprint. It requires patience, consistency, and a willingness to adapt your approach as your body and skin evolve. Remember that there's no one-size-fits-all solution, and what works for one person might not work for another. Integrating professional guidance with your daily holistic practices will yield the most sustainable results. Continually educating yourself and staying attuned to your body's signals are key components of long-term success.
Tackling hormonal acne demands a comprehensive, compassionate approach that acknowledges the intricate connection between your internal health and external skin. By understanding the types of hormonal acne, adopting a targeted skincare regimen, implementing mindful lifestyle choices, and knowing when to seek professional help, you can empower yourself to gain control over your skin. With persistence and the right strategy, clear, healthy skin is not just a dream but an achievable reality.